Arthritis
What Is Arthritis?
Arthritis is a form of joint disorder that involves inflammation in one or more joints. There are over 100 different forms of arthritis.
The most common form of arthritis is osteoarthritis, other forms of Arthritis are rheumatoid arthritis, Septic arthritis, psoriatic arthritis, & related autoimmune diseases.
The major complaint by individuals who have arthritis is joint pain. Pain is often constant, and may be localized to the joint affected.
The pain from arthritis is due to inflammation that occurs around the joint.
Damage to the joint from disease, daily wear and tear of joint, muscle strains caused by forceful movements against stiff painful joints and fatigue
Types of Arthritis
1. Osteoarthritis
Osteoarthritis is a degenerative joint disease, & is a result of trauma to the joint, infection of the joint, or old age.
2. Rheumatoid Arthritis (RA)
Rheumatoid Arthritis (RA) is an autoimmune disease that causes chronic inflammation of the joints
3. Septic Arthritis
Septic Arthritis is also known as infectious arthritis, and is usually caused by bacteria, or fungus.
4. Psoriatic Arthritis
Psoriatic Arthritis is a form of arthritis that affects some people who have psoriasis, a condition that features red patches of skin topped with silvery scales.
5. Autoimmune Diseases
Autoimmune Diseases are a broad range of related diseases in which a person’s immune system produces an inappropriate response against its own cells, tissues and/or organs, resulting in inflammation and damage.
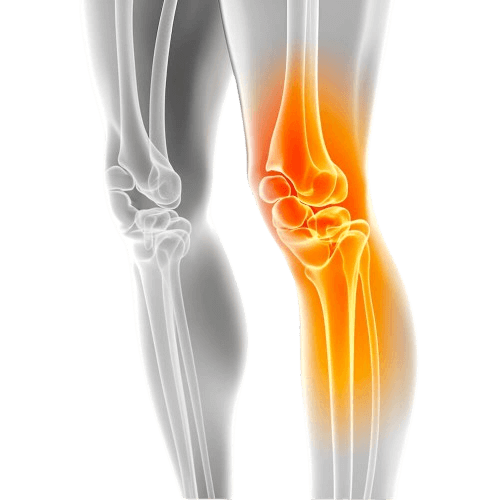


1. Osteoarthritis
Osteoarthritis (OA) is a type of joint disease that results from breakdown of joint cartilage and underlying bone.
Unlike other types of arthritis, only the joints are typically affected. OA is the most common form of arthritis.
Arthritis of the knee and hip affecting about 3.8% of people as of 2010. Among those over 60 years old about 10% of males and 18% of females are affected.
Before 45 years of age it is more common in men, while after 45 years of age it is more common in women. It becomes more common in both sexes as people become older.

Primary Osteoarthritis
A number of studies have shown that there is a greater prevalence of the disease among siblings and especially identical twins, indicating a hereditary basis. Although a single factor is not generally sufficient to cause the disease, about half of the variation in susceptibility has been assigned to genetic factors.
The development of OA is correlated with a history of previous joint injury and with obesity, especially with respect to knees. Since the correlation with obesity has been observed not only for knees but also for non-weight bearing joints and the loss of body fat is more closely related to symptom relief than the loss of body weight, it has been suggested that there may be a metabolic link to body fat as opposed to just mechanical loading.
Changes in sex hormone levels may play a role in the development of OA as it is more prevalent among post-menopausal women than among men of the same age.

Secondary Osteoarthritis
Secondary osteoarthritis (due to an old injury with fracture) of the ankle in a woman of 82 years old
This type of osteoarthritis is caused by other factors but the resulting pathology is the same as for primary osteoarthritis:
2. Rheumatoid Arthritis (RA)
Rheumatoid arthritis (RA) is the most common type of autoimmune arthritis. It is triggered by a faulty immune system (the body’s defense system) and affects the wrist and small joints of the hand, including the knuckles and the middle joints of the fingers.
People have long feared rheumatoid arthritis as one of the most disabling types of arthritis. The good news is that the outlook has greatly improved for many people with newly diagnosed (detected) RA. It still however remains a serious disease, and one that can vary widely in symptoms and outcomes.
Even so, treatment advances have made it possible to stop or at least slow the progression of joint damage. Rheumatologists now have many new treatments that target the inflammation that RA causes. They also understand better when and how to use treatments to get the best effects.
3. Septic Arthritis
Septic arthritis is also known as infectious arthritis, and is usually caused by bacteria, or fungus. The condition is an inflammation of a joint that’s caused by infection. Typically, septic arthritis affects one large joint in the body, such as the knee or hip. Less frequently, septic arthritis can affect multiple joints.
4. Psoriatic Arthritis
Psoriatic arthritis is a form of arthritis that affects some people who have psoriasis — a condition that features red patches of skin topped with silvery scales. Most people develop psoriasis first and are later diagnosed with psoriatic arthritis, but the joint problems can sometimes begin before skin lesions appear.
Joint pain, stiffness and swelling are the main symptoms of psoriatic arthritis. They can affect any part of your body, including your fingertips and spine, and can range from relatively mild to severe. In both psoriasis and psoriatic arthritis, disease flares may alternate with periods of remission.
No cure for psoriatic arthritis exists, so the focus is on controlling symptoms and preventing damage to your joints.
Without treatment, psoriatic arthritis may be disabling.
5. Autoimmune Diseases
Autoimmune Diseases are a broad range of related diseases in which a person’s immune system produces an inappropriate response against its own cells, tissues and/or organs, resulting in inflammation and damage. There are over 80 different autoimmune diseases, and these range from common to very rare diseases.
An autoimmune disease develops when your immune system, which defends your body against disease, decides your healthy cells are foreign. As a result, your immune system attacks healthy cells. Depending on the type, an autoimmune disease can affect one or many different types of body tissue. It can also cause abnormal organ growth and changes in organ function.
There are as many as 80 types of autoimmune diseases. Many of them have similar symptoms, which makes them very difficult to diagnose. It’s also possible to have more than one at the same time. Autoimmune diseases usually fluctuate between periods of remission (little or no symptoms) and flare-ups (worsening symptoms). Currently, treatment for autoimmune diseases focuses on relieving symptoms because there is no curative therapy.
Autoimmune diseases often run in families, and 75 percent of those affected are women.


